The third recurrence of my bowel cancer took the form of a metastasis in my liver and another in my lung. By the end of July 2018, both of these had been successfully removed. Which was awesome. The only fly in the ointment was that the PET/CT scan that I’d had on 5th June revealed a thyroid hotspot…
I hadn’t been worried about the scan, it was just a formality for the thoracic surgeon. It was to make sure that nothing had changed in my lung metastasis, in the time since the liver metastasis had been removed.
So, when I phoned the colorectal nurse specialists, a week later, it was to sort out the timings for the tests related to the lung surgery. What I was told instead, really shook me up. The nurse told me that all timings were now subject to change, because the scan had revealed a thyroid hotspot.
I made note of my thoughts on this development in my journal:
‘[The nurse] told me that these things happen sometimes and that it’s almost always nothing. But, that said, I would need an ultrasound scan and maybe a fine needle aspiration to get a biopsy. Which would need to be done before there can be any thought of surgery.
I told [the nurse] that this had knocked the stuffing out of me and that I didn’t even think thyroid mets were an option. She said that in her 35 years of nursing, she’d never seen a case. This was backed up by a look on the internet. It seems to be a 0.1% occurrence.’
The nurse did her best to be reassuring but it’s tricky to feel reassured when the light at the end of the tunnel turns out to be a train heading your way.

By Hannes Ortlieb (Diskussion) – Own workOriginal text: selbst fotografiert, CC BY-SA 3.0 de, https://commons.wikimedia.org/w/index.php?curid=41678371
The thyroid hotspot was almost certainly unrelated to my bowel cancer. Which was great. But that didn’t mean that I couldn’t also have thyroid cancer…
And, sure, I understand that developing two unrelated cancers before the age of 50 was remarkably unlikely. But, when it came to my experiences with this cancer, I did seem to be something of a shit magnet!
Fortunately a brief bit of research on thyroid cancer showed that survival rates were excellent. My biggest concern became the impact that this development might have on my lung surgery. These concerns were quashed just two days later during my last-minute meeting with the thoracic surgeon. He, too, reiterated that the thyroid hotspot was almost certainly nothing. Which was nice and reassuring. He also pointed out that he’d go ahead with his surgery, whatever the thyroid hotspot turned out to be. Which was just amazing news.
The date for the ultrasound and fine-needle aspiration was 27th June, which rolled around pretty quickly. The most painful part of the process was the injection of local anaesthetic in and around the thyroid. This was needed because the doctor ran the ultrasound wand over my throat and decided he didn’t like the look of the thyroid hotspot. Which meant he needed a sample. Hence the actually painful injection to numb the area.
To be fair, once the anaesthetic kicked in, there was no pain from the actual aspiration. Just a sense of pressure. The doctor used the ultrasound wand to guide the tip of the needle into the right location and then sucked out a sample. this was passed to a Lab Tech, who confirmed that the sample actually contained viable cells. Only then was the needle withdrawn. It seems quite a tricky process to get the tip of the needle in exactly the right place, and this process avoided the potential need to do it twice.
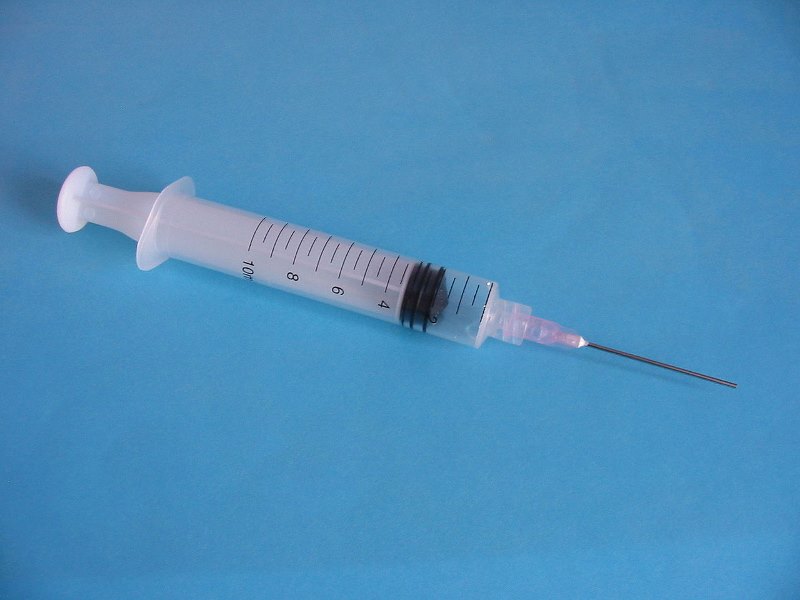
Biggishben~commonswiki assumed (based on copyright claims), CC BY-SA 3.0, https://commons.wikimedia.org/w/index.php?curid=886022
And, when I got home, I appreciated that consideration, because my throat was sore for a good couple of days. It’s strange how such a small needle can cause such a lot of aching…
But, anyway; back to the ultrasound procedure. When he’d finished, I asked the doctor what his first impressions were. As ever, in these circumstances, to get a meaningful answer you have to ask a question that doesn’t require a categorical response. Asking for a ‘first impression’ should elicit a response, because it’s sufficiently vague for the doctor not to worry about getting sued over his response. On which note, if people could stop suing doctors over their answers, that’d be great!
So the doctor said that the cells definitely weren’t from a nice, harmless cyst. They were too dense for that. And they probably weren’t from a tumour; they weren’t dense enough. But if it was a tumour, it definitely wasn’t related to my bowel cancer. The only other thing he was definite about was that the thyroid nodule wasn’t responsible for my excess weight… I’d only said it as a joke!
The impression I was left with was, that while it probably wasn’t cancer, it probably was something. Back to the internet, which revealed two likely candidates:
In reality, though, neither was a good fit and I had other things to think about. The Three Peaks Challenge with Emma, at the end of the month. Oh, and the small matter of my lung surgery on 11th July.
Both of those went well. And, while I was recovering from my surgery, I called after the results of the fine needle aspiration. I was told that nothing was on the system yet and I’d be called back on the 19th July. I found this a little worrying but assumed someone had been on leave. During the call on the 19th, I was told that there was still no news but my case would be discussed during the Multidisciplinary Team meeting (MDT) on the Monday. I’d be called back on Tuesday 24th. Which would be four weeks after the sample was taken, and enough to get me worrying some more.
The call on the 24th introduced me to a brand new expression: ‘follicular proliferation’, and the worry was back in force. The nurse who’d made the call was a colorectal nurse specialist and had no idea what the expression meant. Nor should she; the thyroid is, in a real sense, almost as far from her area of expertise as you can get. Thyroid was an Ear, Nose Throat (ENT) issue, and I’d been referred to them.

Photo by Markus Spiske on Unsplash
In the meantime, it was back to the internet. Searches of ‘follicular proliferation’ returned very little that was definitive. By and large, the expression relates to hair like structures. Which meant that my sample contained hair like structures. The presence of such things seemed to lead down a one-way street that ended in some, or all, or the thyroid gland getting cut out, regardless of whether there was cancer present. It seems that the surgery for a biopsy is sufficiently close to that of a removal, that the removal is done while they’re in there. And not just the thyroid hotspot, the entire half of the thyroid that the hotspot is in.
The other obvious alternative, however, was Follicular Thyroid Cancer…
Fortunately, I didn’t have too long to worry about it because, the very next day, I had my follow up meeting with the thoracic surgeon about my lung surgery. And, as it turned out, he’d done thyroid surgeries in the past. Amazing stroke of luck. ![]()
To his mind, the thyroid hotspot would turn out to be nothing to worry about. Follicular proliferation was simply a way to describe what the Lab Tech saw in the sample, and was not diagnostic. He did, however, confirm that I’d very likely be losing half my thyroid.
Ah, well; sure it would be the third surgery in a year, but at least it’d be somewhere new.
And, finally, my mind was eased sufficiently that I was able to relax a bit. For me uncertainty leads to stress. Too much stress, for too long, leads to depression. I didn’t want to end up depressed again.
My first meeting with the ENT people was on 8th August. The surgeon I spoke to was impossibly young. By which, I mean; he was younger than me. I’d never been operated on by someone younger than me and hoped he’d be doing it. I mentioned this to him, which just left him looking confused…
After which, he stuck a camera up my nose…
This was to get a look at my vocal cords, which were at some risk of being damaged during a surgery on the thyroid. Not directly, but because the nerve for the vocal cords runs under the thyroid. This meant that there was a risk of a change in my voice, which might be temporary or permanent. Or even the loss of my voice, again, potentially permanent. So he wanted to see the vocal cords, hence the camera up the nose.

Photo by Thomas Lefebvre on Unsplash
At least he put a dab of local anaesthetic on the endoscope. Which meant I didn’t feel anything, much less gag. This was a huge relief after my experiences of a tube being put down my throat after my bowel surgery.
The vocal cords must have been fine because he told me I’d be having a hemithyroidectomy. So I would, indeed, be having half of my thyroid cut out, to get rid of the thyroid hotspot. The survival rate was excellent, which was nice. But I might have to take thyroxine tablets thereafter, which was no big deal. And, with that, he packed me off to have my pre-operative assessment.
The date of the surgery turned out to be 10th September. I was having this one done through the NHS, instead of privately as I usually do. There was no real reason for this. The ball got rolling in the NHS while I’d been tied up with my lung surgery. There seemed no point trying to interfere with the situation, so I didn’t.
As such, I checked into the Blake Ward, at Musgrove Park Hospital, at 0800 hrs. Too early for comfort, but at least a ward I’d never been on before. I was scheduled second on the list, meaning I’d be going down at about 1130 hrs. This was enough time to persuade Julie that it was pointless to hang around, so I sent her off to work.
The surgeon came round and explained the procedure. An incision would be made in one of the creases in my neck and the thyroid hotspot, along with the rest of the right half of my thyroid, would be removed through the incision. He then marked up my neck, with permanent marker, to make sure he took the correct half.

By Ivan at en.wikipedia – Own work, Public Domain, https://commons.wikimedia.org/w/index.php?curid=17192013
That’s when I broke out my camera. I explained about my collection of photos from previous operations and asked for one from this one. The gorier, the better. As seems always to be the case, the surgeon looked excited at the prospect and you could see the plans starting to form behind his eyes.
The surgeon, incidentally, wasn’t the younger chap that I’d met on the 8th August. This guy was considerably older than me. On the brighter side of the news, the anaesthetist turned out to be female, which was a first for me.
As with my lung surgery, I actually got to walk into the operating theatre and arrange myself on the operating table. I forget why. But it was nice and airy with a friendly, positive atmosphere. My camera was there and everyone was on board with the photo idea. I went to ‘sleep’ happy. Little did I know that, almost as soon as I was under, a Matron walked in and stamped all over the photo idea. Didn’t matter that it was my idea, on my camera and photos of me. No photos!
Other than that, though, everything went fine. I spent the night in the Ward, where I got about 90 minutes sleep. But that was no problem, because I went home the following day and got some sleep there. There was very little pain from the surgery, or swelling for that matter. Paracetamol dealt with both issues nicely.
I had to wear compression stockings for a couple of weeks. And I would need a blood test and a follow-up meeting shortly thereafter but I’ll mop that up in my next post.
The simple fact was, that the thyroid hotspot was gone. The surgery, my third of the year, had gone really well. And, spoiler alert, the thyroid hotspot would turn out to be completely benign…
2 thoughts on “Thyroid Hotspot During Treatment for Bowel Cancer”
As always an inspiration, your humor in the midst of all this is really inspiring. Wish you a happy new year.
Many thanks.
And a happy New Year to you and your girls.